A US man with terminal heart disease was implanted with a genetically modified pig heart in a first-of-its-kind surgery, and three days later the patient is doing well, his doctors reported on Monday.
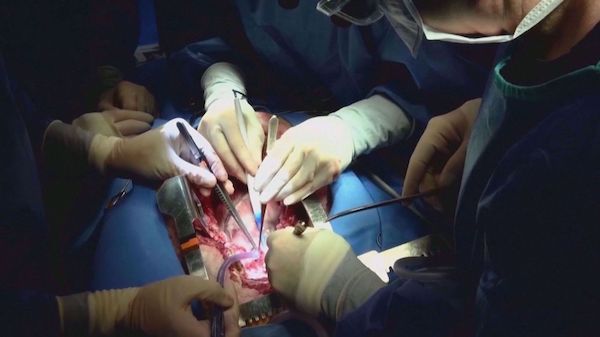
The surgery, performed by a team at the University of Maryland Medicine, is among the first to demonstrate the feasibility of a pig-to-human heart transplant, a field made possible by new gene editing tools.
If proven successful, scientists hope pig organs could help alleviate shortages of donor organs.
"WeÆve never done this in a human and I like to think that we, we have given him a better option than what continuing his therapy would have been," Dr. Bartley Griffith, who surgically transplanted the pig heart into the patient, said in a video interview provided by the university.
"But whether itÆs a day, week, month, year, I donÆt know," Griffith added.
For 57-year-old David Bennett of Maryland, the heart transplant was his last option.
"It was either die or do this transplant. I want to live. I know itÆs a shot in the dark, but itÆs my last choice," Bennett said a day before his surgery, according to a statement released by the university.
To move ahead with the experimental surgery, the university obtained an emergency authorization from the US Food and Drug Administration on New YearÆs Eve through its compassionate use program.
"The FDA used our data and data on the experimental pig to authorize the transplant in an end-stage heart disease patient who had no other treatment options," said Dr. Muhammad Mohiuddin, who heads the UniversityÆs program on xenotransplantation - transplanting animal organs into humans.
About 110,000 Americans are currently waiting for an organ transplant, and more than 6,000 patients die each year before getting one, according to organdonor.gov.
BennettÆs genetically modified pig heart was provided by Revivicor, a regenerative medicine company based in Blacksburg, Virginia. On the morning of the surgery, the transplant team removed the pigÆs heart and placed it into a special device to preserve its function until the surgery.
Pigs have long been a tantalizing source of potential transplants because their organs are so similar to humans. A hog heart at the time of slaughter, for example, is about the size of an adult human heart.
Other organs from pigs being researched for transplantation into humans include kidneys, liver and lungs.
Prior efforts at pig-to-human transplants have failed because of genetic differences that caused organ rejection or viruses that posed an infection risk. Scientists have tackled that problem by editing away potentially harmful genes.
In the heart implanted in Bennett, three genes previously linked with organ rejection were "knocked out" of the donor pig, and six human genes linked with immune acceptance were inserted into the pig genome.
Researchers also deleted a pig gene to prevent excessive growth of the pig heart tissue.
The work was funded in part with a $15.7 million research grant to evaluate RevivicorÆs genetically-modified pig hearts in baboon studies.
In addition to the genetic changes to the pig heart, Bennett received an experimental anti-rejection drug made by Kiniksa Pharmaceuticals based in Lexington, Mass.
(Source: Reuters)
LINK: https://www.ansarpress.com/english/26015
TAGS:




























 MSF reports basic medical needs of Afghans are not being met
MSF reports basic medical needs of Afghans are not being met




